Imagine starting as a new clinic receptionist, and during a staff meeting, your manager mentions scheduling a virtual patient consultation. The term telemedicine pops up, but its meaning escapes you, leaving you unsure how to proceed with the task. This concept is central to modern healthcare delivery, and understanding it is critical for anyone stepping into this field.
By the end of this article, readers will grasp the telemedicine in healthcare definition and its role in daily operations. They will also learn actionable steps to engage with this technology from day one.
- Telemedicine connects patients and providers remotely using technology like video calls.
- It reduces travel for patients, saving time and expanding access to care.
- Clinics use it to manage follow-ups without needing in-person visits.
- Staff must ensure stable internet connections for seamless virtual appointments.
- Administrators track telemedicine billing codes to avoid reimbursement delays.
- Privacy rules still apply — patient data must remain secure during virtual sessions.
- Beginners can start by observing one virtual consultation to see the process live.
What Is Telemedicine in Healthcare?
Telemedicine refers to providing medical care remotely through digital tools like video conferencing or phone calls. For someone new to healthcare management, understanding this concept is vital because it shapes how clinics and hospitals deliver services, especially to patients who cannot visit in person. It is a growing part of operations that impacts scheduling, billing, and patient satisfaction.
Think of telemedicine as a virtual bridge. Just as a physical bridge connects two distant places, telemedicine links a patient in a rural area to a specialist hundreds of miles away via a secure video platform. This connection allows real-time consultations without travel.
Healthcare facilities adopt this approach to increase access to care while managing limited resources. For example, a small clinic with only one doctor on staff can use telemedicine to connect patients with off-site cardiologists for heart-related concerns. Beginners in administration need to recognize how this tool fits into daily workflows, from setting up appointments to ensuring technical support is available.
💼 Healthcare Career Opportunities
Explore healthcare management and administration roles from hospitals, clinics, and health systems.
Browse Jobs →For a deeper understanding of telemedicine, Lean Hospitals: Improving Quality, Patient Safety, and Employee Engagement by Mark Graban covers efficient healthcare delivery methods in plain language suitable for administrators at any level.
How Telemedicine Actually Works
Step 1: Patient Request — The process begins when a patient contacts the clinic for care, often through a phone call or online portal. For instance, a patient with a chronic condition like diabetes might request a follow-up to discuss recent test results without traveling to the facility.
Step 2: Scheduling and Setup — Clinic staff schedule the virtual appointment and send the patient a link or instructions to join via a secure platform. An example is a receptionist confirming a 2 p.m. slot and emailing a video call link to a patient for a dermatology consultation.
Step 3: Technical Preparation — Both the provider and patient ensure their devices and internet are ready before the session. A nurse might test the clinic's webcam and headset an hour before, while the patient logs in early from home using a tablet.
Step 4: Consultation — During the session, the provider assesses the patient, discusses symptoms, and offers advice or prescriptions through the digital interface. A doctor might review a patient's uploaded blood pressure readings during a 15-minute call and adjust medication accordingly.
Step 5: Follow-Up and Billing — After the session, staff document the visit in the patient's record and process insurance claims with specific telemedicine codes. A billing clerk in a rural clinic, for example, submits claims to ensure reimbursement, referencing guidelines from the AHA for accurate coding.
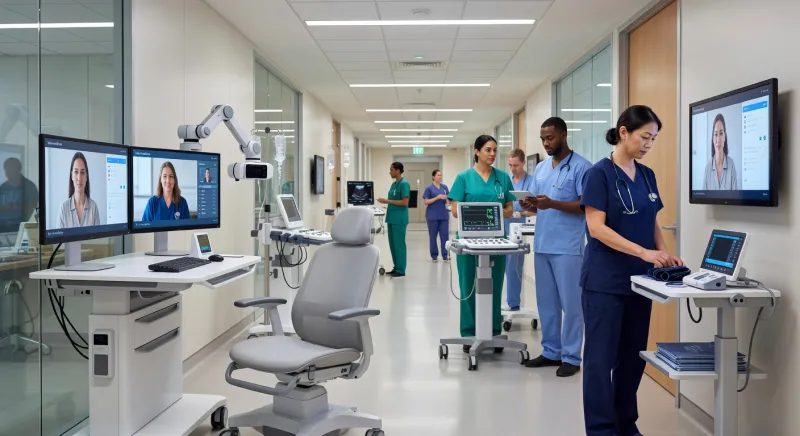
Key Roles in Telemedicine Operations
Several roles in a healthcare facility handle telemedicine to ensure smooth delivery. Each contributes uniquely to the process, and understanding their tasks helps beginners see where they fit. Here are the primary players involved.
First, receptionists manage the initial patient interaction. They schedule virtual appointments and send access instructions, often confirming a patient's tech readiness a day before the session. Their role keeps the process organized from the start.
Next, clinical staff, such as nurses, often assist during consultations. They might join a call to take notes or upload vital signs like a patient's weight into the system during the session for the doctor's review.
Then, IT support staff maintain the technical backbone. They troubleshoot connection issues, ensuring a provider can conduct a video call without interruptions by testing systems daily.
Finally, billing specialists handle the financial side. They code virtual visits correctly for insurance, reviewing claims each week to prevent denials due to errors in documentation.
Common Challenges in Telemedicine
New administrators often face hurdles when dealing with remote healthcare delivery. Identifying these issues early can prevent bigger problems. Below are three common challenges and practical solutions.
First, technical difficulties disrupt sessions. Patients or staff may struggle with unstable internet or unfamiliar software, leading to delayed or canceled appointments. A fix is to create a simple one-page guide on joining virtual calls and distribute it during scheduling.
Second, privacy concerns arise with digital interactions. Sharing patient information over unsecured networks risks violating regulations like HIPAA — the federal law protecting health data. Staff can address this by using only approved, encrypted platforms, following standards from The Joint Commission.
Third, reimbursement issues complicate billing. Insurers may reject claims if telemedicine codes are incorrect or if documentation lacks detail, delaying payments. A practical approach is for billing staff to double-check codes against payer policies before submission, reducing errors upfront.
Practical Starting Points for New Administrators
Newcomers to healthcare management can take actionable steps to get familiar with remote care delivery. These tasks build confidence and understanding. Here are five starting points to try.
1. Observe a virtual consultation session to see the flow from patient login to provider interaction.
2. Review the clinic's digital platform user guide to understand basic navigation and troubleshooting tips.
3. Ask the IT team for a quick demo on securing patient data during online sessions.
4. Request a copy of the telemedicine billing codes used by the facility to recognize common entries.
5. Explore additional resources on remote healthcare through the Telemedicine section for broader insights.
Frequently Asked Questions
What is telemedicine in healthcare?
Telemedicine in healthcare refers to delivering medical services remotely using digital tools like video calls or phone consultations. It allows patients to consult with providers without visiting a facility, often for follow-ups or minor issues. For example, a patient might discuss medication adjustments with a doctor via a secure app from home, saving travel time and reducing clinic overcrowding.
How does telemedicine benefit patients?
Telemedicine offers patients convenience by eliminating the need for travel, especially for those in rural areas or with mobility issues. It also provides faster access to specialists who may be far away. A patient with a skin rash, for instance, can show it to a dermatologist over video within days instead of waiting weeks for an in-person slot.
What technology is needed for telemedicine?
Telemedicine requires a device like a smartphone, tablet, or computer with a camera and microphone, plus a stable internet connection. Secure software or apps approved by the healthcare facility are also essential. For example, a clinic might use a dedicated platform to ensure patient data remains private during a virtual mental health session.
Are telemedicine visits covered by insurance?
Many insurance plans cover telemedicine visits, but coverage depends on the provider, state laws, and specific services rendered. Clinics must use correct billing codes to ensure reimbursement. A small practice might confirm with a patient's insurer beforehand to avoid surprise out-of-pocket costs for a routine virtual check-up.
What are the limitations of telemedicine?
Telemedicine cannot handle emergencies or conditions requiring physical exams, like setting a broken bone. Technical issues or lack of internet access can also hinder sessions. For instance, a doctor cannot perform a hands-on assessment of abdominal pain over video and may require the patient to visit in person for accurate diagnosis.
Readers now understand what telemedicine means in healthcare and how it integrates into daily clinic operations. They have learned its process, key roles, and common pitfalls alongside practical ways to engage with it.
Start today by asking a supervisor to let you observe one virtual patient consultation — even 10 minutes of watching the interaction reveals how remote care connects patients and providers in real time.
